 June 9, 2025
June 9, 2025May Image Of The Month
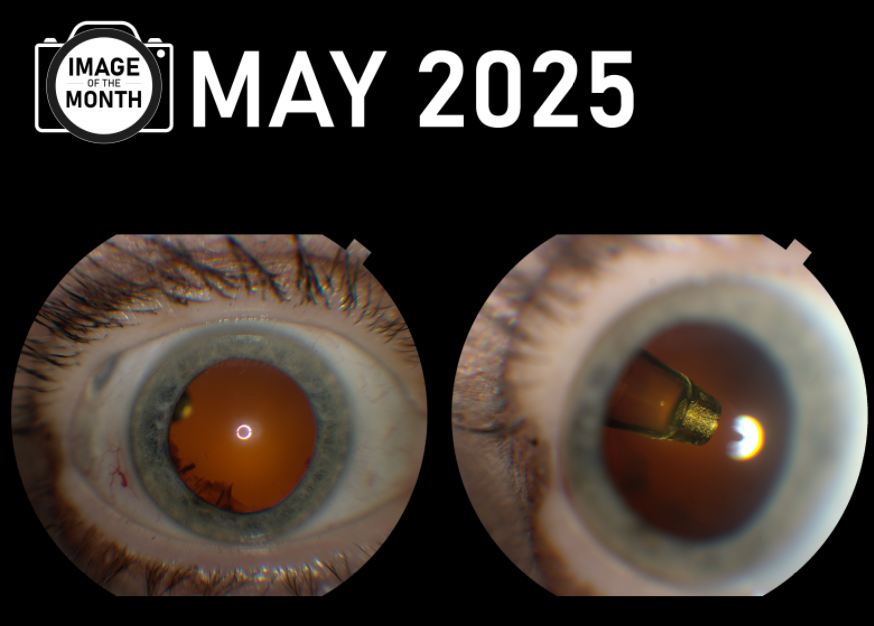
Dezirae Elkins captured the Image of the Month for May of the FDA approved Port Delivery System (PDS). This delivery system is a surgical procedure used to …
![]() May 26, 2025
May 26, 2025April Image Of The Month
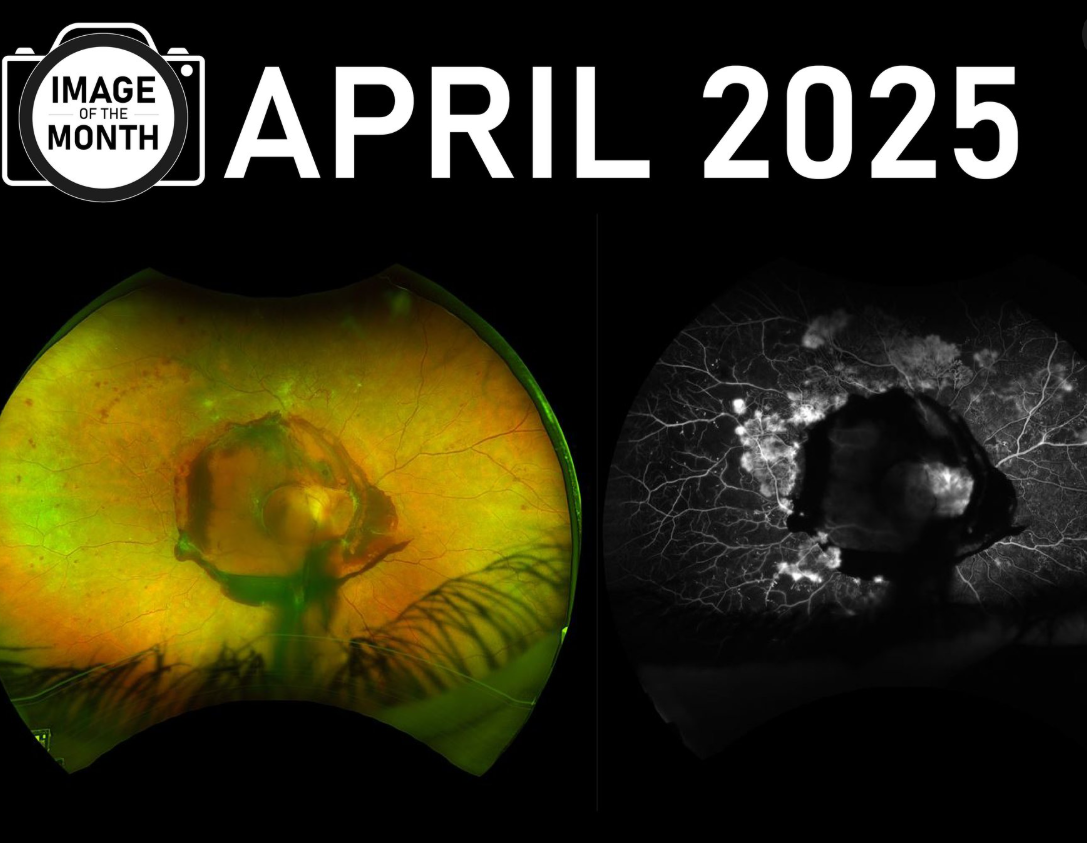
Rebekah Greenberg captured the TNR Image of the Month for April of a Large Pre Macular Hemorrhage. This kind of hemorrhage is related to a large pool of blood …
![]() May 5, 2025
May 5, 2025March Image of the Month
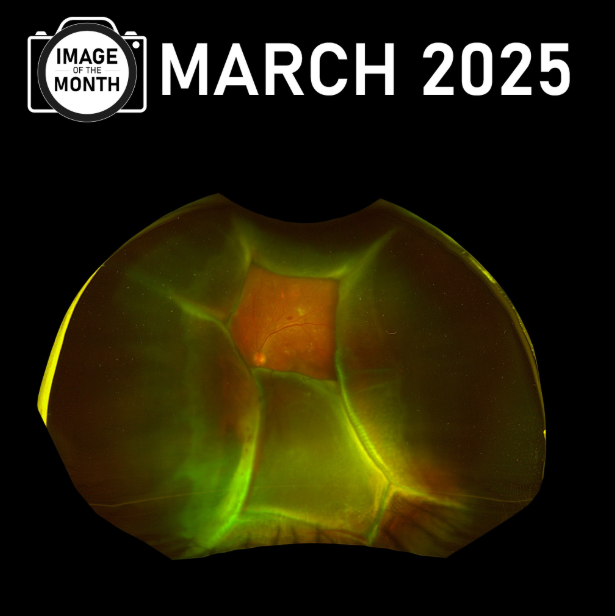
Kaitlyn Anderson captured the TNR Image of the Month for March of a Choroidal Detachment on our OPTOS camera. Choroidal detachment occurs when there is fluid …
![]() April 23, 2025
April 23, 2025When to See a Doctor About Eye Flashes and Floaters
Posted on December 30, 2024 • by RCA • in RCA Featured Blog Posts Many people with healthy eyes will occasionally see flashes and floaters in their field of …
![]() March 17, 2025
March 17, 2025Save Your Vision & American Diabetes Alert Day
Save your vision month and American diabetes alert day are both recognized in March. We encourage you to always be mindful and on top of checking your vision …
![]() March 10, 2025
March 10, 2025February 2025 Image of the Month
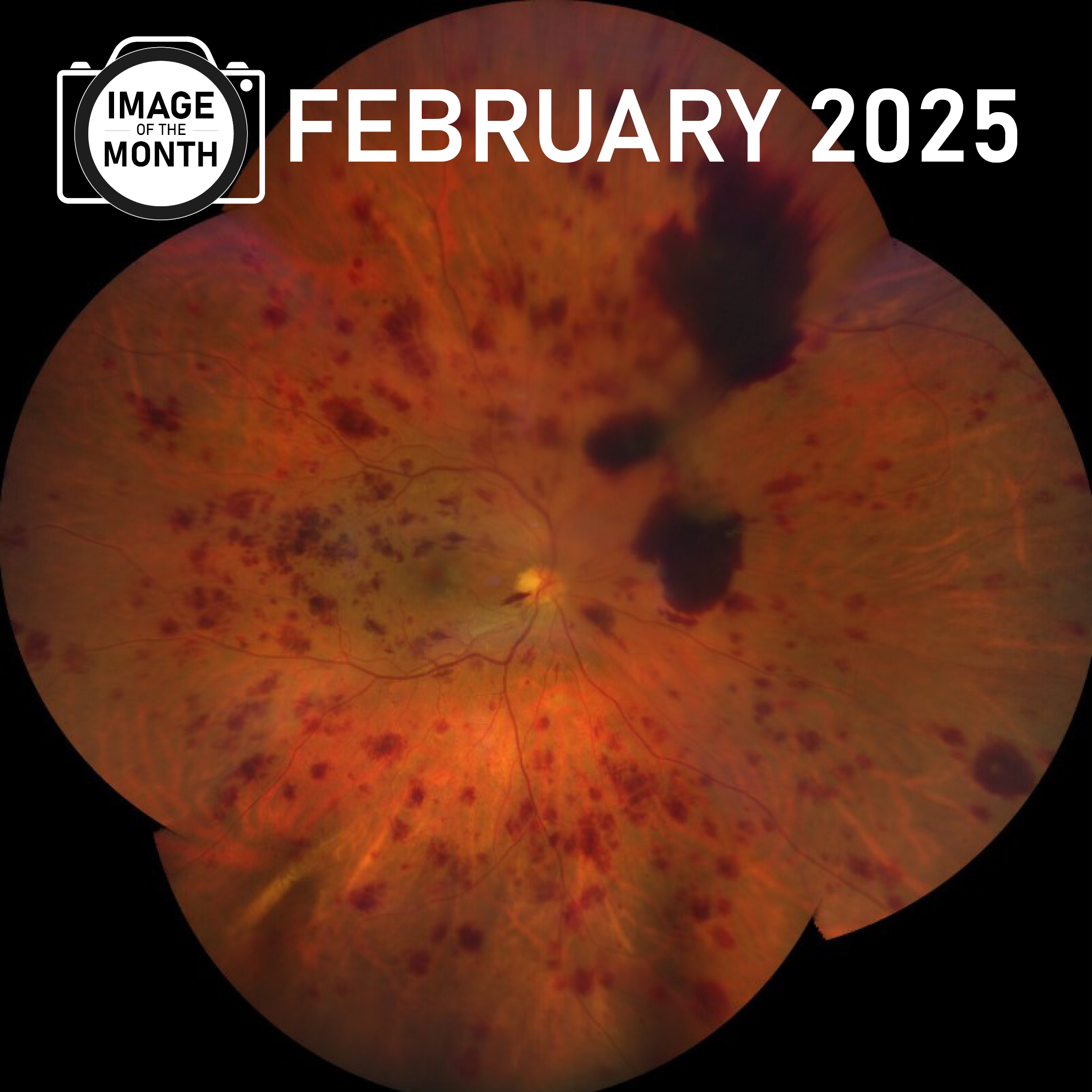
Nicole Knight is the winner of the photo of the month for February! Congratulations Nicole!! Diagnosis: PDR OD and severe NPDR OS Camera: Clarus Findings: …
![]() February 24, 2025
February 24, 2025Jan 2025 Image of the Month
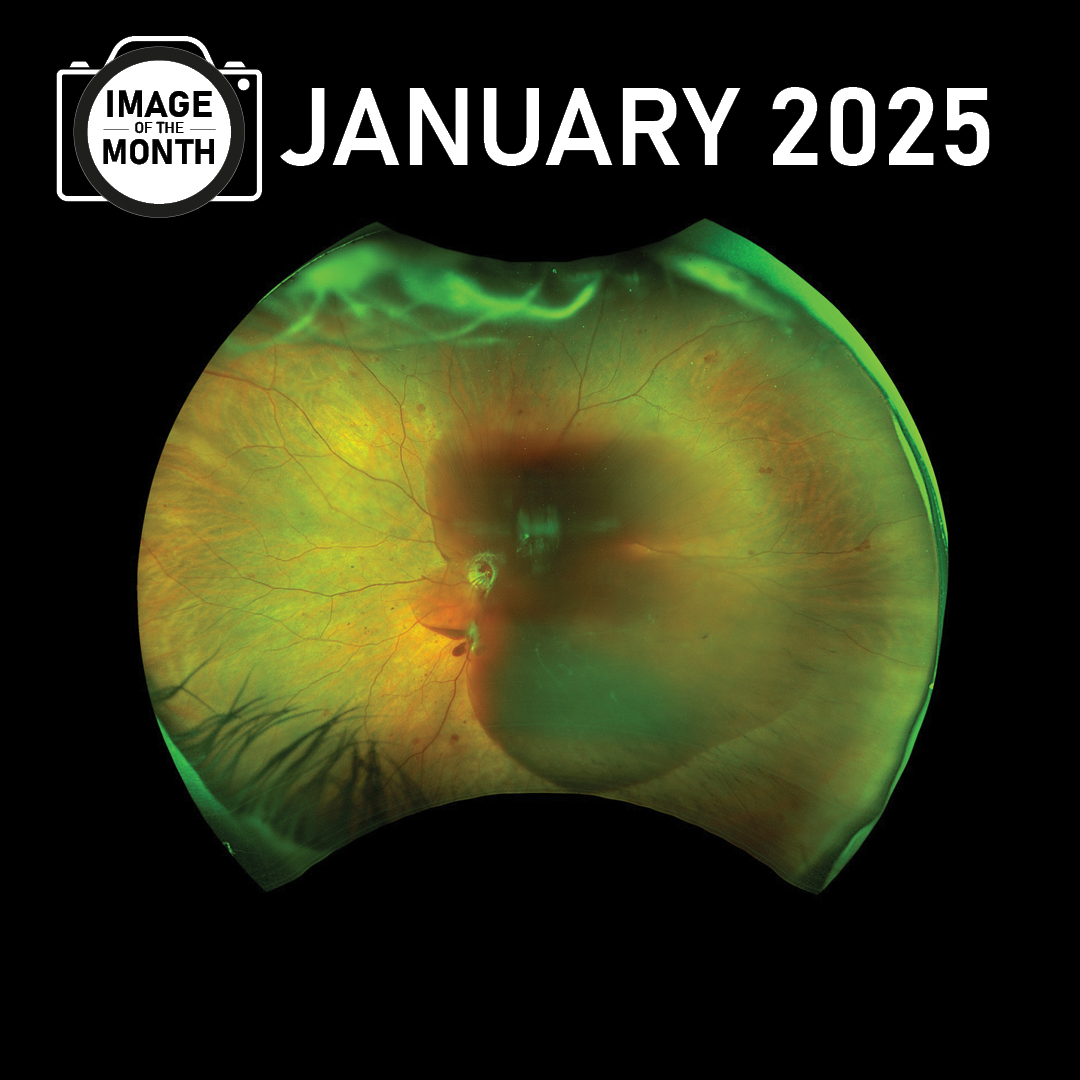
Our incredibly talented TNR photography team submit images each month and vote on their favorite. We are happy to announce that Hollie Sanders is the winner of …
![]() February 19, 2025
February 19, 2025February is AMD and Low Vision Awareness Month
February is AMD and Low Vision Awareness Month. We encourage you to always be mindful of the importance of checking your vision at home. Early detection is …
![]() January 15, 2025
January 15, 2025Joy Award 2024
Named in loving memory of TNR employee Angie Joy Huddleston, this award is presented annually by the practice to the individual who is consistently attentive …
![How to Maintain Healthy Retinas as You Age]() December 2, 2024
December 2, 2024How to Maintain Healthy Retinas as You Age
Posted on September 3, 2024 • by RCA • in RCA Featured Blog Posts Vision changes are a natural part of the aging process. However, there are ways to help …
Blog Search
Follow TNR
Categories
- AMD & Low Vision
- American Diabetes Alert Day
- Blog
- Diabetes
- Firework Eye Safety
- Health & Wellness Expo 2024
- Risks of smoking and AMD
- Stroke
- Women's Eye Health & Safety Month
Tags
- A1C
- Age Related Macular Degeneration
- AMD
- American Diabetes Alert Day
- Amsler Grid
- Appointment Request Form
- babies
- Blog
- Blood Sugar Monitoring
- BowlingGreenKY
- Checking Vision At Home
- ChoroidalDetachment
- Coats' Disease
- Diabetes
- Diabetes Awareness
- Dr Recchia
- eyes
- Eye Safety Fireworks New Year 4th of July
- Flashes&Floaters RCA TNR RetinaDoctors
- Foresee Home Monitoring
- FreeHealthScreenings
- gestational age
- Glucose
- Health&Wellness
- HealthierYou
- image of the month
- Joy Award
- Laser
- Low Vision
- March2025
- pediatric retina
- Protective eye wear
- Quality Staff
- Quit Smoking
- retina
- Risks of Smoking
- ROP
- Save Your Vision
- Smoking
- Sun
- sunscreen
- Support Group
- TNR
- TNR Research
- Ultraviolet rays
- Vitreoretinal Consultants of NY
- Women Macular Degeneration Cataracts Diabetics Health screening living longer
Welcome to the TNR Blog! Here, we offer patients essential information and insights into the world of retinal health. Check back here often to stay up-to-date on all things retina as well as important announcements from our practice.
Get the Exceptional Care You Need